10th anniversary Mbale’s world class maternal and neonatal research centre
The Sanyu Africa Research Centre (SAfRI) is a world-class research centre that focuses on maternal and newborn health. Since being registered ten years ago, it is going from strength to strength.
Origins
The founding organisations for SAfRI were the Ministry of Health, Uganda; Makerere University; Busitema University; Mbale Regional Referral Hospital; and the University of Liverpool in the UK. It is celebrating the tenth anniversary of its registration this month.
A globally significant research centre
Although SAFRI was set up as an NGO (non-government organisation) by the founding organizations, it is not under the control of any one of them but is an independent, flexible research centre. It enables all interested parties to have an impact on maternal and child health not only locally, or within Uganda, but globally through its association with organisations around the world such as GYNUITY Health Projects in the USA; the Medical Research Council (MRC) in the UK; and the European & Developing Countries Clinical Trials Partnership (EDCPT) in the European Union.
Its latest project is the BabyGel study, which tests the effectiveness of alcohol-based handrub to protect newborn infants from infection. The handrub is produced from sugarcane at the local Kakira Sugar works. Six thousand families living in 72 villages in Eastern Uganda have been part of the study and it is due to complete this month.
SAFRI was named after Mrs Edith Sanyu, a woman from Mbarara who died in childbirth in 2012. She had travelled to Kampala to Mulago Hospital when she developed severe complications in her pregnancy. Although not well known herself, she represents the many people who suffer daily through the lack of resources for maternal and child health. The meaning of the name (translated as ‘joy’) is also important as SAfRI is hoping to bring happiness through its activities.
Highlights of its history include:
Exchange partnerships between UK and Uganda
For further details please contact Dr Benon Wanume, SAfRI Executive Director
THE ORIGINS OF SAFRI
Background
The founder of SAfRI, Andrew Weeks, is Professor of International Maternal Health Care at the University of Liverpool. He was brought up in Kenya and trained as a doctor in obstetrics and gynaecology in the UK, returning to East Africa to take up a post of visiting lecturer at Makerere University in 2001, From 2005-7 he was chief investigator for the ‘Release Study’ on the treatment of retained placentas. This study ran in 13 sites in 3 countries, including Mulago Hospital and Mbale Regional Referral Hospital, and was published in the Lancet in 2010.[1]
In 2006 the clinical link with Makerere University and Mulago Hospital was formalized when Professor Weeks set up the Liverpool-Mulago Partnership to facilitate staff exchanges between the two units. This charity ran from 2007 until 2017.
In 2010 funding was obtained from the Bill and Melinda Gates Foundation / Gynuity Health Projects to set up MamaMiso, a community study looking at new ways of preventing bleeding after childbirth. The study ran in Mbale district and tested the benefits of giving a drug called misoprostol to women in pregnancy so that they could take it themselves after birth.
Formation of the Sanyu Research Unit in 2011, Liverpool
Meanwhile, Professor Weeks and colleagues formed a research centre in Liverpool called the Sanyu Research Unit. MamaMiso was part of its work.
Formation of the Sanyu Africa Research Institute (SAfRI) in 2013, Uganda
The MamaMiso study ran through 2012 and 2013, and a young nurse called James Ditai was employed by the University of Liverpool to run the study. As part of the study setup he was asked to also set up the Mbale branch of Sanyu, which they called the Sanyu Africa Research Institute (SAfRI). The first chair of the board was Professor Weeks, but with his close involvement in all the research, he resigned to make place for someone more independent. And so, in 2015, Professor Florence Mirembe took over and she has been the chair of SAfRI since then. Professor Mirembe is Emeritus Professor, Makerere University, College of Health Sciences, and Professor at Uganda Christian University in the Faculty of Science and Technology.
Group photo from the official launch of SAfRI in January 2014. Source: SAfRI
MAMAMISO
MamaMiso was the first SAfRI project, a trial set up in 2008 on preventing women from bleeding after childbirth.
Dr John Baptist Waniaye Nambohe, the commissioner for Emergency Medical Services, Ministry of Health, was involved with the SAFRI MamaMiso trial from its start, when he was the District Health Officer for Mbale.
“The first SAFRI activity that helped to change Ugandan health policy on the care of mothers was the MamaMiso study,” Dr Nambohe said.
“MamaMiso proved that misoprostol was a superior drug, safe and effective in preventing and managing the bleeding of women after childbirth.
“The mothers who benefited from the study expressed their gratitude and were always willing to participate because of the friendliness of the attending midwives and doctors.
“Meanwhile the capacity of the researchers was enhanced by their participation in SAFRI activities.
“Altogether the contribution to the national policy guidelines for management of bleeding after childbirth was a great contribution by SAfRI.”
In 2013, Sarah Nerima chats with a SAfRI researcher outside of her house, four days after childbirth. The research team provided misoprostol tablets to pregnant women for self-administration immediately after giving birth to prevent bleeding. Sarah is holding the ‘MamaMiso purse’ which contained the study tablets along with a picture-based instruction sheet. Source: SAfRI
For more details on the MamaMiso study please follow this link: https://bmcpregnancychildbirth.biomedcentral.com/articles/10.1186/s12884-015-0650-9
LIVERPOOL-UGANDA EXCHANGE PARTNERSHIPS
Over the last decade, 94 Ugandan and British doctors, midwives and administrators have been on exchange visits between hospitals in Uganda and Liverpool. It started with the Liverpool-Mulago partnership but later extended to other hospitals in Uganda. Funding mainly came from the British Commonwealth Scholarship exchange partnership scheme. The Fellows spent time in working with their exchange partners in each country, undergoing training courses, and setting up development plans.
Dr Nambohe was also a Fellow of the scheme. “I participated in the Commonwealth Scholarship exchange partnership scheme in which I learnt a lot in terms of good clinical practice, clinical research and health leadership and governance,” Dr Nambohe said.
“The exposure contributed to my promotion to Ministry of Health as a Commissioner of Emergency Medical Services. I remain grateful.”
Fellows from Mbale visiting Liverpool in 2013. Source: SAfRI
For more details on the partnership please follow this link: https://www.bmj.com/content/342/bmj.d64
BABYSAVER
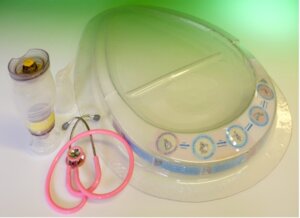
The BabySaver kit was designed in Liverpool and developed with Ugandan midwives. It is a low-cost, portable package that brings together all the equipment needed for helping newborn babies into one package. It needs no electricity, and keeps the mother, newborn and midwife together during the critical period immediately after the birth.
The BabySaver kit. Source: SAfRI
It was created by a team of experts led by Professor Andrew Weeks and designed with Peter Watt, an engineer from Royal Liverpool and Broadgreen University Hospitals NHS Trust. Prototypes were manufactured at Bryn Y Neuadd Hospital in Gwynedd, Wales.
“Each year approximately six million babies across the world require basic neonatal resuscitation and around 900,000 of these will die,” Professor Weeks said.
“The vast majority of deaths occur in low-income settings where there are few facilities for newborn resuscitation at birth.
“Where resuscitation does occur, it often happens away from the mother – or even in another room, which can be very distressing for the mother and baby.
“The BabySaver enables resuscitation to take place at the bedside, with the umbilical cord still attached.
“Allowing the cord to stay intact has huge health benefits for newborn babies but it also allows the midwife to stay with the mother at a high risk time for her.”
SAfRI has the rights for its use in Africa. Meanwhile, the BabySaver kit is being developed for use all over the world; this year it is also being produced to send to the war-torn areas of Europe.
For more details on the BabySaver trolley, and its sister the LifeStart trolley, please follow these links
https://safri.org/the-baby-saver/
https://www.bbc.co.uk/news/uk-wales-45485604
https://bmcpediatr.biomedcentral.com/articles/10.1186/1471-2431-14-135
https://www.liverpoolwomens.nhs.uk/news/first-hospital-in-uk-to-introduce-bedside-neonatal-care/
BABYGEL
Infectious diseases are a huge cause of child death; the BabyGel trial was set up in 2019 to see if using an alcohol-based handrub in rural households helps to reduce infection for newborn babies and their mothers. The handgel is made in Uganda using locally-sourced sugar cane, so it supports local farmers and Ugandan industry as well.
The BabyGel study is recruiting 6000 participants from hard-to-reach communities in 72 villages in the Mbale District of Eastern Uganda. Women are given a “Maama” birth kit to be used at births, and advice on hygiene. Women in half of the villages are also given enough handrub for the first three months after they have had their baby. If the trial proves successful, the handrub could be included in delivery packs for every expectant mother in Uganda.
Outreach on the BabyGel project. Source: SAfRI
Dr Agnes Napyo, honorary lecturer at Busitema University, is a researcher in the BabyGel study.
“The study supports not just mothers, but those in the community who are involved in making sure that optimal maternal and newborn health is achieved – village health teams, midwives, nurses, boda boda transporters, community leaders, and members of the media,” said Dr Napyo.
“For instance, the boda boda transporters have reported to us that they have been explaining the importance of BabyGel to men. This has helped to increase the involvement of men in the project, not just the mothers.”
For more details on the BabyGel study, please follow these links
https://sanyuresearch.org/BabyGel/
https://trialsjournal.biomedcentral.com/articles/10.1186/s13063-023-07312-1
Dr Napyo has conducted research interviews with those involved with BabyGel: for quotes from these interviews please see below.
Infant sepsis is a life-threatening condition that can develop fast in babies who have an infection. This is a BabyGel group meeting on infant sepsis in Busiu. Source: A. Napyo
From mothers:
“I went to the BabyGel offices when my baby was sick. I spent a week in the hospital… the BabyGel doctor kept checking on me and my baby and requested for treatment change. The doctor also gave me and my baby all the money that we required for upkeep. We eventually returned to Nakaloke as outpatients and the midwife treated us so well.”
“I thank the BabyGel project, especially for the mama kit. My husband could not afford to buy a mama kit.”
“I benefited a lot from BabyGel. When one gets a problem, one is taken care of very well.”
From spouses:
“My wife got a mama kit and other things from BabyGel. When the time of delivery approached, I called the health worker who came immediately and I was happy.”
“I am happy with the BabyGel project. My child was helped. I was given transport for my child when he was sick.”
From midwives:
“I thank the project for the follow-up it does for the mothers and babies. We don’t follow up these mothers in the Ministry, but BabyGel has helped in this.”
“I thank BabyGel for bringing for us a blood pressure machine at the health facility which we did not have.”
From boda boda riders:
“We benefit from BabyGel just like the health workers do, we also get paid. Thank you BabyGel.”
“I have witnessed by myself that the project is beneficial. When a mother or baby is sick, the health workers care for you very well.”
From religious leaders:
“I keep seeing these health workers following up mothers. They have also helped to improve hygiene in our homes.” – Pastor / village health team member (a pastor who also works as a VHT)
“I am very thankful to the project because it has it has influenced the increase of hygiene in the home. When the health worker came, he toured around our home and this made us to become more cautious of the hygiene.” – Imam (Muslim religious leader)
From village health team members:
“Some women when they have a sick child, they don’t have money; but BabyGel will pay the transport. Even when they are referred to hospital, they are followed up.”
“I thank BabyGel for following up on mothers. The health workers are very diligent. BabyGel should continue.”
“The help the women get from the facility for their babies especially for women of advanced age that get pregnant is great. These women fear the way that they will be treated at the hospital, so BabyGel has encouraged the elderly women to deliver in the hospital.”
[1] Weeks et al., Umbilical vein oxytocin for the treatment of retained placenta (Release Study). Lancet 2010;375:141-47]. https://pubmed.ncbi.nlm.nih.gov/20004013/